Radiation Treatment in the 1950s on Babies Born With Enlarged Thymus Glands
- Research
- Open Admission
- Published:
Risk of coronary events 55 Years after Thymic irradiation in the Hempelmann cohort
Cardio-Oncology volume 4, Article number:1 (2018) Cite this article
Abstract
Background
Studies of cancer survivors treated with older radiotherapy (RT) techniques (pre-1990s) strongly propose that ionizing radiation to the chest increases the chance of coronary heart disease (CHD). Our goal was to evaluate the impact of more than modernistic cardiac shielding techniques of RT on the magnitude and timing of CHD take chances by studying a cohort exposed to similar levels of cardiac irradiation years ago.
Methods
Betwixt 2004 and 2008, we re-established a population-based, longitudinal cohort of 2657 subjects exposed to irradiation for an enlarged thymus during infancy betwixt 1926 and 1957 and 4388 of their non-irradiated siblings. CHD events were assessed using a mailed survey and from causes of expiry listed in the National Death Index. We used Poisson regression methods to compare incidence rates by irradiation status and cardiac radiation dose. Results were adjusted for the CHD risk factors of attained-age, sex, diabetes, dyslipidemia hypertension and smoking.
Results
Median age at time of follow-up was 57.five years (range 41.2–88.8 yrs) for irradiated and non-irradiated siblings. The hateful estimated cardiac dose amongst the irradiated was 1.45 Grey (range 0.17–20.20 Gy), with 91% receiving < 3.00 Gy. During a combined 339,924 person-years of follow-up, 213 myocardial infarctions (MI) and 350 CHD events (MI, bypass surgery and angioplasty) occurred. After aligning for attained age, gender, and other CHD take a chance factors, the rate ratio for MI incidence in the irradiated grouping was 0.98 (95%CI, 0.74–i.xxx), and for any CHD event was one.07 (95%CI, 0.86–1.32). College radiation doses were non associated with more MIs or CHD events in this dose range, in either the crude or the adjusted analyses.
Conclusions
Radiations to the heart during childhood of < three Gy, the exposure in well-nigh of our accomplice, does not increment the lifelong risk of CHD. Reducing cardiac radiation to this amount without increasing other cardiotoxic therapies may eliminate the increased CHD risk associated with radiotherapy for childhood cancer. Past extension in that location is unlikely to be increased CHD chance from relatively higher dose imaging techniques, such every bit CT, because such techniques use much smaller radiation doses than received by our cohort.
Introduction
Since the late 1980s several studies of cancer survivors treated with older chest radiotherapy techniques have demonstrated that they are at increased risk of cardiac bloodshed and morbidity [1,ii,iii,iv,v,6,7,viii]. Childhood cancer survivors who received mediastinal radiotherapy are particularly at high chance for coronary heart disease (CHD) [9,10,11], and as a consequence, radiotherapy techniques accept been modified to reduce the dose and book of the heart exposed to irradiation (east.k. shielding the heart, limiting daily fraction size, lower total doses). However such modifications have been relatively recent and so the impact on cardiovascular wellness during adulthood remains uncertain. Although lower-dose volumes of exposure are thought to not increase risk, studies of populations exposed to lower doses of whole body irradiation such as the atomic bomb survivors have reported an increased risk of cardiovascular morbidity and mortality, only not necessarily from CHD specifically [12,13,xiv,xv], with the exception of i historical accomplice of individuals treated at the University of Chicago for peptic ulcers [xvi].
In the start one-half of the previous century, a misconception of the normal size range of thymus glands in infants and the mistaken belief that an enlarged thymus could lead to status lymphaticus and suffocation [17, 18] led to thousands of infants and children being irradiated for thymic enlargement. In 1951, Louis Hempelmann began a longitudinal cohort to report cancer incidence among patients treated for this condition in Rochester, NY, between 1926 and 1957 and their untreated siblings [xix, 20]. The re-initiation of this dormant accomplice allowed the states to gauge the effect of more modern techniques of chest radiotherapy for childhood and boyish cancer on coronary heart illness incidence and mortality over nigh of the lifespan. This is considering although this cohort was treated with older techniques, they received total cardiac doses similar to the cumulative doses many children with cancer receive with more than modernistic RT techniques. Additionally since the cardiac doses this cohort received is twenty to 500 times greater than that received for a chest computed tomography (CT), this study may inform the higher end of lifetime cardiac risk of children who receive multiple CT scans [21, 22].
Methods
The population-based Hempelmann cohort
This population based cohort and survey methods are described in more detail in elsewhere [23, 24]. In brief, the accomplice was formed in the early and mid 1950s by collecting records from all Rochester, New York, area hospitals and clinics, that administered thymic irradiation, except for one practise that closed in 1944 and whose records were destroyed. (This clinic treated fewer than 400 children.) All exposed subjects received orthovoltage irradiation. The number of fractions ranged from one to 7, although 89% of patients received but one or two treatments. Time between the outset and last treatment was xc days or less for 98% of patients; 96% were treated at 1 year of age or less. Non-irradiated siblings built-in before the 3rd follow-up survey in 1963 were included in the cohort. Subjects were excluded if follow-up ended within 5 years later on birth, either from death or loss to follow-upwards [20]. The studied cohort included 2657 thymic irradiated and 4833 non-thymic irradiated siblings, referred to as the irradiated and not-irradiated siblings, respectively, or subjects collectively, throughout the rest of the paper. Irradiated individuals had a variable number of siblings, including none at all, so straight matching comparisons could not be easily performed.
The cohort was surveyed past mail or telephone half-dozen times, between 1953 and 1987 [xix, twenty, 25,26,27,28], merely these surveys did not collect information related to cardiovascular illness, except whether the respondent smoked. Survey response rates were high and similar among irradiated and not-irradiated siblings. In the 1985 survey, approximately 85% of both groups responded; 5% had died, and 10% declined to participate or were lost to follow-up.
Data collection
Cardiac dosimetry
In the early on 1990s, Dr. Stovall and colleagues re-estimated the radiation doses to various organs of each subject, and for the get-go time estimates were calculated for the heart. The method of dose estimation is described in an earlier publication [24], and used information bathetic from the original patient records including cumulative air dose to the thymus, historic period at each handling, treatment field size, thickness of atomic number 82 protection, kilovoltage, and position of treatment (posterior, anterior, or both). The dose reconstruction methods used are similar to those used in other similar cohorts [29, 30]. Only 4.7% had insufficient data to judge cardiac dose and were classified as "cardiac dose unknown." Three subjects had received other radiation treatments concurrently with thymic irradiation. Their doses for this analysis are based solely on their thymic irradiation.
Recent follow-up procedures
We re-initiated follow-up of this cohort in 2003 every bit described previously [24]. Briefly, cohort members were eligible for follow-up if they had returned whatsoever of the before surveys. During the first year of updating contact data prior to sending out whatever surveys, nosotros adamant that about xi% of the accomplice had died and another 10% were non locatable.
Between 2004 and 2008, we collected self-reported data using an 81-item survey. The survey collected data on outcomes and adventure factors for cardiovascular disease and cancer. Upwards to three mailing attempts and four telephone calls were made to each subject.
Data on CHD chance factors were collected primarily in the 2004–2008 survey. However, the 1985 survey also assessed smoking status and hypothyroidism. Subjects who reported having had a myocardial infarction (MI), coronary artery intervention or angina were sent a medical release form so nosotros could obtain relevant medical records. Records were reviewed by two of 4 preventive cardiologists/physicians (TAP, RGS, RB, MJA) on a blinded, independent basis in order to determine if a subject field had one or more coronary heart disease event(s) reported by the patient or side by side of kin. Reviewers used the Centre Outcomes Prevention Evaluation Group diagnostic criteria for MI [31]. Along with MI, documented angioplasty and coronary artery bypass were considered to exist CHD events, but angiography without treatment and angina without intervention or MI were not. Discrepancies in reviewers' assessments were resolved past consensus between the two physicians who reviewed a subject field's record.
CHD outcomes were also assessed with crusade of death information from the National Death Alphabetize (NDI) on the years between its start in 1979 and 2005. MI was divers equally ICD9 codes 410–12 and ICD10 I21–24. CHD was defined past the post-obit codes ICD9 codes 410–414, 427.v and ICD10 codes I21-I25, I46. Up to the outset five causes of death listed were analyzed. Nosotros used NDI cause of death data to ostend events reported by next of kin in the electric current survey, but we did not seek further confirmation of events reported past the NDI solitary because of the difficulty in obtaining medical records for these events.
Statistical methods
We hypothesized that subsequently adjusting for known take a chance factors, low-dose therapeutic chest radiation would increase the life-long cumulative incidence of MI and CHD, as compared to non-irradiated siblings. We also determined the excess relative risk and excess absolute risk of MI and CHD per Greyness (Gy) after adjusting for other CHD take chances factors in our sample.
To calculate person-years at risk, we used date of nativity as the beginning date for both irradiated and not-irradiated siblings, considering 95% of the exposed had been irradiated past 8 months of historic period. Thus, length of follow-upwardly is nearly equivalent to age at follow-up. The event date was the date of CHD event; data were censored at the about recent survey response. Date of death was only used every bit an terminate date if that was the only date nosotros had for an incident CHD issue, if that was the last follow-up information nosotros had on the subject (censoring date), or if we received a survey subsequently from next of kin (censoring date or used date of CVD event provided by next of kin).
Incidence rates and their 95% confidence intervals (95% CI) were calculated by irradiation status and dose groups, from which charge per unit ratios adjusted for sex and attained age and their 95% CI were calculated [32]. Potential CHD risk factors and demographic variables (attained age, sex, always smoked, history of diabetes mellitus, history of dyslipidemia, history of hypertension, and family history of MI and/or sudden decease) were compared past thymic irradiation status using Student's t-examination for continuous variables and Pearson'south chi-foursquare examination for chiselled variables. Dyslipidemia was defined equally self-reported high cholesterol, loftier LDL cholesterol and/or loftier triglycerides on the 2004–8 survey. Data conformed to the assumptions of the tests used to analyze them. These analyses were performed using SAS version 9.2. Multivariate assay included only subjects who responded to all CVD gamble and events questions on 2004–8 survey, i.e. no information imputation methods were used for missing information.
For categorical dose and excess relative take a chance modeling, we performed multivariate Poisson regression using the AMFIT module in the Epicure statistical program [33, 34]. All statistical tests addressing our main hypotheses were ii-sided with an alpha level of 0.05. Person-years were calculated from nascence as described above and cantankerous-classified by calendar year, a time-dependent variable of attained historic period, sexual activity, heart radiation dose, and potentially significant CHD run a risk factors in our cohort. Model fit was evaluated using two-sided likelihood ratio tests at the v% significance level [35]. Likelihood-based 95% conviction limits were calculated when possible. Reported charge per unit ratios for the entire accomplice were adjusted for those factors that were significant in our most parsimonious models for MI and all CHD events respectively.
Excess relative risk was modeled with respect to the cardiac radiation dose. A typical excess relative chance model used to evaluate linear-dose and dose-squared components was:
$$ \mathrm{ERR}=\uplambda \mathrm{south}\ \exp\ \left(\sum {\alpha}_j{x}_j\right)\ \left(1+{b}_1D+{b}_2{D}^two\right) $$
Where ERR is the excess relative take a chance of MI/CHD, λs is model stratum baseline rates of MI (or CHD) events (strata by sex and attained age) based on the rates in the non-irradiated siblings, the exponential term teni represents potentially significant independent risk factors for MI (or CHD events and αi represents their individual coefficient estimates. D represents the estimated cumulative center radiations dose in Gy, and βone and βtwo represent the coefficientsof consequence size for the dose terms.
Results
MI/CHD incidence
A full of 3071 subjects, 1303 irradiated and 1768 non-irradiated siblings responded to the current survey, for an overall response rate of 46%, after excluding those known to take died (Table 1). Of these responders, 990 irradiated and 1368 not-irradiated siblings had complete data on CHD risk factors and CHD outcomes. Median historic period at follow-up of was 57.5 years (range, 47.5–78.3 years) in the irradiated and 57.five years (range, 41.2–88.viii years) in the not-irradiated siblings. Median estimated cumulative middle exposure was i.41 Gy (range, 0.17–twenty.2 Gy; mean 1.45 Gy) amidst all irradiated individuals in the cohort. The frequency of CVD risk factors differed between sibling groups but for sex and hypothyroidism (Tabular array 2), although each of the CVD risk factors, except hypothyroidism, were significantly associated with having an MI (Table iii).
Myocardial infarction occurred in 83 irradiated individuals suffered an MI and 130 non-irradiated siblings over 126,513 and 213,411 person-years respectively (Table 4). The resulting crude rate ratio for MI later on thymic irradiation was 1.08 (95%CI, 0.82–1.42). Adjusted for attained age and sex, the rate ratio betwixt exposed and unexposed siblings became ane.02 (95%CI, 0.77–one.34) (Tabular array 4). After adjusting for the other nerveless CHD gamble factors the adjusted rate ratio cruel further to 0.98 (95%CI, 0.74–1.thirty) (Tabular array 4). The seventh cavalcade in Table 3 illustrates the charge per unit ratios for all the unlike variables in this fully adapted model of CHD incidence.
Among irradiated individuals, 144 had a CHD event (MI, coronary artery intervention or angina) as did 206 non-irradiated siblings over 126,244 and 213,024 person-years respectively (Table 5). (Person-years of follow-up vary slightly, considering the commencement CHD event appointment may differ outset MI date.) The resulting crude rate ratio for a CHD event after thymic irradiation was 1.17 (0.94–1.39). Adjusting for attained age and sex gave a rate ratio of 1.12 (95%CI, 0.xc–i.39), and 1.07 (95%CI, 0.86–1.32) after adjusting for the other collected CHD risk factors as well (Table 5). The last column in Table 3 illustrates the rate ratios for all the different variables in this fully adjusted model of CHD incidence.
Dose event modeling
Modeling ERR as a linear function over the entire follow-upwardly catamenia resulted in an backlog relative risk per Greyness (ERR/Gy) for MI of − 0.05 (95%CI, − 0.thirteen – 0.08) or − 5% (95%CI, − 13 – 8%) later excluding the individuals with an unknown cardiac radiation dose and adjusting for attained age and sex (Fig. 1a). Adjusting for other CHD adventure factors, the ERR/Gy was − 6% (95%CI, − 16 – six%) (Fig. 1b). The linear dose model did not fit the data improve than a model without dose (likelihood ratio test, p = 0.42), nor did the linear-quadratic (p = 0.27) or quadratic models (p = 0.09) fit meliorate than a linear dose model.
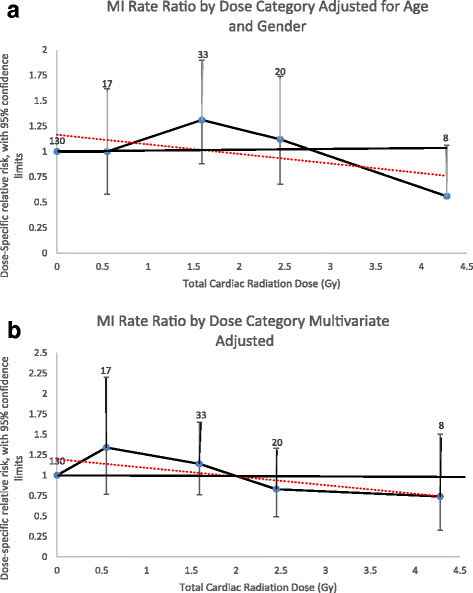
Myocardial Infarction Charge per unit Ratios by Radiation Dose Category. a Adapted for attained historic period and sex only. b Multivariate adjusted (attained age, sex, diabetes, dyslipidemia, ever smoked, and hypertension). Rate ratios plotted by mean dose of intervals evaluated. Number equals number of events for individuals exposed to that dose category. Dotted line equals linear regression line the slope of which is the ERR/Gy estimate
Estimates obtained for the combined CHD events incidence analyses differed. The ERR/Gy for CHD was eight% (95%CI, − 1 – 20%) in a linear dose model adjusted for attained age and sexual activity (Fig. 2a). This linear dose model did not fit the data better than a model without dose (likelihood ratio test, p = 0.08). The linear-quadratic (p = 0.11) and quadratic models (p > 0.fifty) also did not fit the data amend than the linear dose model. The linear model adjusted for all significant CHD risk factors revealed an ERR/Gy of − iii% (95%CI, − 7 – x%) (Fig. 2b).
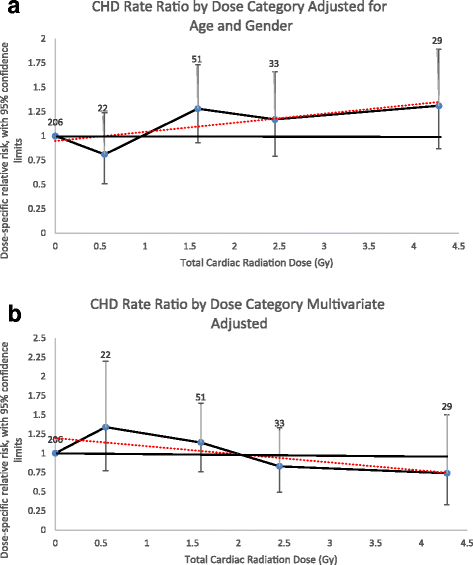
Coronary Artery Disease Effect Rate Ratios by Radiation Dose Category. a Adjusted for attained historic period and sex only. b Multivariate adapted (attained historic period, sex, diabetes, dyslipidemia, ever smoked, and hypertension). Rate ratios plotted past mean dose of intervals evaluated. Number equals number of events for individuals exposed to that dose category. Dotted line equals linear regression line the gradient of which is the ERR/Gy gauge. Coronary avenue disease events include myocardial infarction, coronary avenue featherbed surgery and angioplasty
Give-and-take
Although therapeutic doses of irradiation that includes the center in the treatment field increase the lifelong take chances of cardiovascular disease, and particularly coronary eye disease [ane,two,3,4,5,6,7,8, 36, 37], our results point that breast irradiation in the range we studied, mostly 0 to3 Gy during early childhood, is unlikely to markedly increase long-term CHD gamble in the individual. This dose range is two to three magnitudes greater than that of a chest CT scan, which is typically 7 mGy [21, 22, 38] but one order of magnitude lower than the cumulative doses given for Hodgkin Disease (25 – 40Gy).
Although nosotros constitute no meaning linear dose response, which appears to contradict with the findings of other investigators, our point approximate for ERR/Gy for the incidence of CHD of 8% (95%CI, − 1 – 20%) is really consistent with what others have plant. This is true whether we compare our estimates to those from cohorts exposed to moderate- to depression-level, whole torso irradiation (atomic bomb survivors and nuclear workers) or to outdated therapies for benign diseases or cancer.
Since we conceived of this study, in 2002, Little et al. published a meta-analysis (8 studies; 635,000 people followed for every bit long as 53 years) summarizing information on the circulatory affliction risks associated with moderate- and low-level, whole-body irradiation (a hateful cumulative dose less than 0.5 SV and a daily dose rate less than 10mSV per day) [39]. They estimated an increased relative hazard per sievert (ERR/Sv) of 10% (95%CI, v% – fifteen%) for ischemic centre illness (IHD), using a fixed effects, no-threshold, linear dose model.
Among the studies included in the meta-analysis past Little et al., two studies evaluated diminutive bomb survivors. The first evaluated a smaller group of about xx,000 serially followed survivors (the Adult Health Study population) for cumulative incidence of CHD based on follow-up until 1998. Information technology revealed an backlog relative gamble for IHD incidence of 4% (95%CI, − 6 – fourteen%) per Sievert [xl]. The estimate for MI specifically was 11% (95%CI, − x – 46%), which overlaps with our estimate. Interestingly in survivors less than 40 years old at the time of the bombing, radiation dose was significantly associated with MI incidence, with an ERR/Sv of 25% (95%CI, 0–69%). However, this upshot was for a quadratic dose human relationship. This finding caused us to test quadratic and linear-quadratic dose models besides as linear dose models.
In the second study, published in 2010, Shimizu et al. [13] evaluated circulatory affliction mortality upwardly through the end of 2003 in 86,611 Atomic bomb survivors in the Life Span Report performed. They establish that a linear model fit overall heart disease all-time with an ERR/Sv of 14% (95%CI, 6–23%) when calculated over the entire dose range of exposure (< 0.005–two.00+ Sv). However the relationship was no longer statistically meaning when the analysis merely included survivors with doses less than 0.5 Gy. For IHD specifically, the ERR/Gy was ii% (95%CI,-10–15%), a finding non entirely consistent with a linear dose result model nor statistically pregnant. The inability of this assay to demonstrate significant ERR/Gy for IHD, emphasizes that very big studies with long follow-upwardly periods are sufficiently powered to detect a statistically significant result of lower doses of irradiation to the heart.
A study quite like to ours evaluated CHD incidence in patients treated for peptic ulcer affliction with radiotherapy or other ways between 1936 and 1967 at the Academy of Chicago. Using dose estimates calculated past the same group that performed our dose estimates (Stovall et al.), Carr et al. [16] reported a dose dependent increase in CHD bloodshed after an boilerplate follow-up of 22.v years in the 1475 irradiated patients and 27.v years in the 1568 non-irradiated subjects and subsequently adjusting for several factors including sexual activity and historic period at treatment. Irradiated patients received average full cardiac doses ranging from 0.1 to seven.6 Gy delivered typically in daily fractions of ane.5 Gy during 1 or two half-dozen- to 14-day treatment courses. The hazard of CHD showed no signs of elevation (RR = 1.00 (95%CI, 0.76–i.33)) in the quarter of patients with cardiac doses less than 2.0 Gy, which is interesting because that the average cumulative dose of cardiac irradiation in our cohort was but ane.45 Gy. In 2012, Little et al. evaluated the ERR models for CHD mortality in the Carr study and found an ERR/Gy of 10.ii% (95%CI, 3.nine–17.4%), after adjusting for the two CHD gamble factors, smoking and alcohol utilise, for which they had information [41].
Two more contempo studies have evaluated the linearity of CHD mortality with increasing dose in patients irradiated for beneficial disease. Zablotska et al. evaluated IHD mortality in the Canadian Fluoroscopy Accomplice Study that included 63,707 tuberculosis patients exposed to multiple fluoroscopic procedures (mean lung dose, 0.79 Gy; range, 0–11.sixty Gy) between 1930 and 1952 and followed for causes of decease from 1950 to 1987, for a full of 1.9 million person-years [42]. Although the overall risk of death from non-cancer causes was significantly lower in this cohort than in the general Canadian population (p < 0.001), the ERR/Gy of lung irradiation for IHD mortality was 17.six% (95%CI, 1.one–39.iii%) after adjusting for dose fractionation. In the smaller Massachusetts tuberculosis fluoroscopy cohort with xiii,568 persons, exposed to a mean lung dose of 0.36 Gy (range 0–8.56 Gy) between 1915 and 1968, the linear relationship between lung irradiation and IHD mortality was negative, at an ERR/Gy of − vii.7% (95%CI, − thirteen – one.2%) [43], a similar finding to ours. Not surprisingly, with respect to the studies discussed and so far, the Massachusetts cohort is most similar to ours in terms of person-years of follow-upward and second virtually like ours in term of cumulative dose of exposure, second only to the larger Canadian study. Both studies used lung doses which can be slightly lower or up to 2 times lower than the respective cardiac dose [44]. Also of interest is, that in the Canadian cohort, fourth dimension since therapy was associated with a decreasing upshot of radiation on IHD bloodshed, whereas in studies of childhood cancer survivors and in our study time since therapy or attained age independently increased the hazard of IHD mortality equally discussed below. Quite recently a pooled analysis of these studies was performed [44]. It plant that the ERR/Gy for IHD was 27% (95%CI, 0.iii–55%) when analyses were restricted to doses < 0.5 Gy simply negative − iv% (95%CI -half-dozen – -1%) over the entire range. Indeed for virtually all circulatory outcomes, the ERR/Gy estimate was greater the more restricted the dose range analyzed, though the biological basis for such restrictions is not definitive.
Several studies in the last decade have evaluated the ERR/Gy curve for CVD in cancer survivors. Tukenova et al. studied the long-term mortality in 4122 v-year survivors of a childhood cancer diagnosed before 1986 in France and the United Kingdom. Cardiac dose averaged five Gy (range 0 - >15Gy) [45]. After an average follow-upward of 27 years, the ERR/Gy for all cardiac mortality was sixty% (95%CI, 20–250%) after adjusting for sexual activity, historic period at treatment, duration of follow-upward, and other factors. However the increased run a risk was not statistically significant in the categorical evaluation of dose until exposure was five.0 Gy or greater. Mulrooney et al. performed similar analyses of CVD incidence in fourteen,358 v-yr survivors and 3899 siblings in the Babyhood Cancer Survivors Report surveyed repeatedly between 1994 and 2002 [46]. In addition to increased risk for all CVD outcomes combined, there was a dose-dependent increase in MI incidence, even after adjusting for known CVD adventure factors and other cancer therapy factors. The average mean cardiac dose in those irradiated was about 12 Gy (range < 0.i - > 35.0 Gy). The specific ERR/Gy for the incidence of MI in this cohort was 4.five% (95%CI, 1.0–8.9%) This estimate was non noted in the original newspaper, just it was reported past Darby et al. in the word of their population-based, case-control study of major coronary events (i.e. MI, coronary revascularization, or expiry from IHD) in 2168 women who underwent radiotherapy for breast cancer between 1958 and 2001 in Sweden and Denmark [37]. The boilerplate, whole cardiac dose was 4.nine Gy (range, 0.03–27.72 Gy). Incidence rates of major coronary events increased linearly cardiac dose [ERR/Gy of 7.four% (95%CI, ii.nine to xiv.5%)], with no apparent threshold.
Comparing our findings to others is complicated by several reasons. In the low-dose studies reviewed past Little et al. in 2012 [39], the exposures were whole-body exposures and, with the exception of the atomic bomb survivors, were at a very low dose rates over a long catamenia. Thus, the rest of pathological mechanisms causing different forms of CVD is probable to be different than in our population [47,48,49]. Additionally, some of the studies discussed used effective doses (Sieverts) in their evaluations, whereas we used absorbed doses (Gray) to the heart. Although with gamma-rays and X-rays these units should be equivalent, the difference does make comparisons confusing. Even when absorbed doses were used, doses to unlike target organs were used for modeling ERR, such equally in the TB studies which used lung doses. In comparing our study to those in cancer survivors, our accomplice's boilerplate cardiac dose (and dose range) was much lower, though more than similar in that treatment was targeted. On the other manus the outcome of cardiac irradiation on CHD in cancer survivors is confounded and likely increased by dysregulation of inflammation from cancer and its treatment with other agents.
Strengths and limitations
The most notable limitation of our written report is its dependence upon self-report and national death records to obtain information on CHD incidence. Besides the potential shortcomings of such data in terms of accuracy, this dependence also limited our ability to observe CHD deaths before 1970, the starting time of the NDI, and in non-respondents to the 2004–2008 survey, given that information technology was the but survey to ask about CHD incidence. The express ability to detect events in earlier years is mitigated by the fact that CHD incidence increases with historic period, being fairly uncommon at less than 40 years of age.
Regarding the accuracy of self-reported data, among participants for whom we could obtain medical records, 65% of self- reported MIs that were confirmed to accept occurred at the reported time and another 13% had evidence for a probable MI or prior MI. Because we only obtained medical records from a minority of those reporting an MI or CHD event, nosotros did not formally integrate confirmation information into our analyses.
Another issue is that we may have underestimated the absolute incidence rates of events by including person-years during which we could not have detected an effect. We included the person-years of non-respondents to the 2004–2008 survey up until their last survey response among the prior surveys, fifty-fifty though these questionnaires did not ask about CHD. Withal nosotros performed analyses that started follow-upwards from age 15 year because the first cocky-reported case of CHD occurred at age 16 years, which helps minimize these potential actress person years; the results were remarkably consistent (data non shown). The issues related to upshot ascertainment and computing person-years of follow-upwardly should have afflicted both irradiated and non-irradiated siblings equally leading to not-differential bias. Further, the result of radiation on heart affliction was likely not well known among the general population at the time our survey. Additionally, our survey asked almost multiple outcomes without stating that our main involvement was CHD; prior questionnaires did not inquire about the occurrence of CHD at all.
Some other limitation of the report is the adequately depression response charge per unit in the 2004–2008 survey which differed between the irradiated and non-irradiated siblings. Given the lower response in non-irradiated siblings, if annihilation we virtually likely underestimated the rate of the disease in this comparison group, thus overestimating any effect of irradiation. Yet, we establish little result at the doses to which our cohort was exposed. Additionally, in an earlier article on thyroid cancer using factors collected in the 1985–1987 survey, nosotros evaluated whether this response pattern might lead to differential non-response bias, threatening internal validity [23]. Of the 13 factors compared, the only CHD risk factors that significantly differed between responders and non-responders for merely one grouping were smoking and hypothyroidism. Smoking was underrepresented in the not-irradiated sibling respondents (54.7% vs 61.7%, p < 0.001), and hypothyroidism was overrepresented in the irradiated individuals (6.0% vs. 3.9%, p = 0.026).
Finally our outcome mixed CHD incidence and mortality. Radiation probably acts through separate withal overlapping mechanisms to increment incidence and mortality, which may differ by exposure levels [48]. The get-go mechanism increases inflammation in the coronary arteries, enhancing the development of coronary atherosclerosis. The latter mechanism increases inflammation in the cardiac microcirculation damaging the heart and causing any age-related MI to be more lethal even if the frequency of coronary ischemia is the same. Arguably, these mechanisms propose that lower irradiation exposures could increase the lethality of MI and CHD without increasing the incidence. Nosotros studied primarily incidence whereas the studies most like to ours studied mortality, and so the to a higher place might assistance explicate why our issue size differs from almost previous studies.
Our study has several strengths. First, to our cognition, the median time since irradiation in the Hempelmann Cohort is longer than that of any other radiation-exposed cohort followed for cardiovascular disease, other than the atomic bomb survivors' cohort [13] and parts of the Massachusetts tuberculosis cohort [43]. Second, in our written report, the sibling comparison group helps control for confounding from family history and potential risk factors that were not collected but are related to upbringing. Third, although the radiation received past our accomplice differs from that used today in terms of dose distribution and less-precise techniques, it is more than similar to the therapeutic and diagnostic radiation received by patients today than is the whole-torso radiation received by diminutive flop survivors or occupationally exposed cohorts. Fourth, our cohort was exposed during childhood and not adulthood, every bit were nearly of the exposures in the tuberculosis cohorts and the entire peptic ulcer disease cohort. Finally, radiation was not administered in response to cancer, so our findings are not confounded by the possibility that an initial malignancy or other therapies increased the risk of coronary middle affliction.
Conclusions
We did not find a significant effect of therapeutic breast irradiation during childhood in the dose range studied (cardiac dose, generally 0 - 3Gy) on the cumulative incidence of CHD or MI upward to an average of 57.five years subsequently exposure. At worst, with such exposures over the life-span, the risk of a CHD outcome is increased by vii%, although this increase is neither statistically significant nor clinically of import compared to the risks imposed by traditional cardiovascular disease run a risk factors. This finding, and the existing literature on childhood cancer survivors, suggests that limiting cardiac exposures to such depression therapeutic doses without increasing other cardiotoxic therapies might eliminate the increased gamble of CHD from chest irradiation for childhood cancer treatment. Additionally. because exposures in our cohort were about 200 times college than that for a breast or abdominal CT in children, our results suggest relatively higher dose imaging techniques such every bit CT, is unlikely to increase CHD take chances.
Nonetheless, our estimated 8% (95% CI, − 1% to 20%) excess relative run a risk per Gy of cardiac irradiation on the incidence of CHD is consistent with what others have found regarding IHD mortality and incidence, though the latter has been studied less. In other radiation exposed cohorts, whether of diminutive bomb survivors, those exposed to radiations for benign diseases, or cancer survivors, estimates of ERR/Gy for IHD have ranged from − 7.7% to 17.six% with the all-time fit generally beingness a no-threshold, linear-dose model. Thus although our results did not fit a linear dose model with statistical significance, our findings also do non provide substantial evidence to abnegate such a model. This is because our estimates are rather consistent with the literature, and the relatively smaller size of our study leads to less precise estimates.
Abbreviations
- CHD:
-
Coronary heart disease
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- CVD:
-
Cardiovascular disease
- ERR:
-
Backlog relative adventure
- Gy:
-
Gray (standard unit of absorbed irradiation)
- ICD:
-
International Classification of Diseases (ICD-9 or − 10, International Classification of Diseases, Ninth Revision or 10th revision)
- IHD:
-
Ischemic heart disease
- MI:
-
Myocardial infarction
- NDI:
-
National Decease Index
- Sv:
-
Sievert (standard unit of effective irradiation) For gamma rays and x-rays 1 Sv = 1 Gy)
References
-
Mauch PM, Kalish LA, Marcus KC, Shulman LN, Krill Due east, Tarbell NJ, et al. Long-term survival in Hodgkin's disease: relative impact of mortality, second tumors, infection and cardiovascular affliction. Cancer J Sci Am. 1995;one:33.
-
Hoppe RT. Hodgkin'due south disease: complications of therapy and excess mortality. Ann Oncol. 1997;8(Suppl 1):115.
-
Hancock SL, Tucker MA, Hoppe RT. Factors affecting belatedly mortality from centre disease after handling for Hodgkin's illness. JAMA. 1993;270:1949.
-
Cuzick J, Stewart H, Rutqvist L, Houghton J, Edwards R, Redmond C, et al. Crusade-specific mortality in long-term survivors of breast cancer who participated in trials of radiotherapy. J Clin Oncol. 1994;12:447.
-
Cuzick J, Stewart H, Peto R, Baum G, Fisher B, Host H, et al. Overview of randomized trials of postoperative adjuvant radiotherapy in breast cancer. Cancer Treat Reports. 1987;71:15.
-
Rutqvist LE, Johansson H. Mortality past laterality of the primary tumor among 55, 000 breast cancer patients from the Swedish centre registry. Br J Cancer. 1990;61:866.
-
Rutqvist LE, Lax I, Fornander T, Johansson H. Cardiovascular mortality in a randomized trial of adjuvant radiations therapy versus surgery lone in primary breast cancer. Int J Radiat Oncol Biol Phys. 1992;22:887.
-
Adams MJ, Hardenbergh PH, Constine LS, Lipshultz SE. Radiation-associated cardiovascular disease. Crit Rev Oncol Hematol. 2003;45:55.
-
Hancock SL, Donaldson SS, Hoppe RT. Cardiac disease post-obit treatment of Hodgkin's disease in children and adolescents. J Clin Oncol. 1993;11:1208.
-
Swerdlow AJ, Higgins CD, Smith P, Cunningham D, Hancock BW, Horwich A, et al. Myocardial infarction mortality risk after treatment for Hodgkin disease: a collaborative British cohort study. J Natl Cancer Inst. 2007;99:206.
-
Ng AK, Bernardo MP, Weller E, Backstrand KH, Silver B, Canellos GP, et al. Long-term survival and competing causes of expiry in patients with early stage Hodgkin's disease treated at age fifty or younger. J Clin Oncol. 2002;xx:2101.
-
Preston DL, Shimizu Y, Pierce DA, Suyama A, Mabuchi One thousand. Studies of mortality of atomic bomb survivors. Report 13: solid cancer and noncancer disease mortality: 1950-1997. Radiat Res. 2003;160:381.
-
Shimizu Y, Kodama K, Nishi N, Kasagi F, Suyama A, Soda M, et al. Radiation exposure and circulatory affliction risk: Hiroshima and Nagasaki diminutive bomb survivor data, 1950-2003. BMJ. 2010;340:b5349.
-
Azizova TV, Muirhead CR, Druzhinina MB, Grigoryeva ES, Vlassenko EV, Sumina MV, et al. Cardiovascular diseases in the cohort of workers first employed at Mayak PA in 1948-1958. Radiat Res. 2010;174:155.
-
Azizova TV, Muirhead CR, Moseeva MB, Grigoryeva ES, Vlasenko EV, Hunter N, et al. Ischemic heart affliction in nuclear workers first employed at the Mayak PA in 1948-1972. Health Phys. 2012;103:3.
-
Carr ZA, State CE, Kleinerman RA, Weinstock RW, Stovall K, Griem ML, et al. Coronary center disease afterwards radiotherapy for peptic ulcer disease. Int J Radiat Oncol Biol Phys. 2005;61:842.
-
Friedlander A. Status lymphaticus and enlargement of the thymus with written report of a instance beingness successfully treated by x-ray. Arch Pedatri. 1907;24:491.
-
Saenger EL, Silverman FN, Sterling TD, Turner ME. Neoplasia following therapeutic irradiation for benign conditions in babyhood. Radiology. 1960;74:889.
-
Simpson CL, Hempelmann LH, Fuller L. Neoplasia in children treated with X-rays in infancy for thymic enlargement. Radiol. 1955;64:840.
-
Shore RE, Hildreth N, Dvoretsky P, Andresen E, Moseson M, Pasternack B. Thyroid cancer amidst persons given X-ray treatment in infancy for an enlarged thymus gland. Am J Epidemiol. 1993;137:1068.
-
Mettler FA Jr, Huda W, Yoshizumi TT, Mahesh K. Effective dose in radiology and diagnostic nuclear medicine: a itemize. Radiol. 2008;248:254.
-
Miglioretti DL, Johnson Eastward, Williams A, Greenlee RT, Weinmann S, Solberg LI, et al. Pediatric computed tomography and associated radiation exposure and estimated cancer risk. JAMA Pediatr. 2013;167:700.
-
Adams MJ, Shore RE, Dozier A, Lipshultz SE, Schwartz RG, Constine LS, et al. Thyroid cancer risk 40+ years after irradiation for an enlarged thymus: an update of the Hempelmann cohort. Radiat Res. 2010;174:753.
-
Adams MJ, Dozier A, Shore RE, Lipshultz SE, Schwartz RG, Constine LS, et al. Chest cancer take chances 55+ years after irradiation for an enlarged thymus and its implications for early on childhood medical irradiation today. Cancer Epidemiol Biomark Prev. 2010;nineteen:48.
-
Pifer JW, Toyooka ET, Murray RW, Ames WR, Hempelmann LH. Neoplasms in children treated with Ten-rays for thymic enlargement. I Neoplasms and mortality J Natl Cancer Inst. 1963;31:1333.
-
Hempelmann LH, Pifer JW, Burke GJ, Terry R, Ames WR. Neoplasms in persons treated with x rays in infancy for thymic enlargement. A report of the tertiary follow-up survey J Natl Cancer Inst. 1967;38:317.
-
Hempelmann LH, Hall WJ, Phillips 1000, Cooper RA, Ames WR. Neoplasms in persons treated with 10-rays in infancy: quaternary survey in twenty years. J Natl Cancer Inst. 1975;55:519.
-
Shore RE, Woodard E, Hildreth N, Dvoretsky P, Hempelmann L, Pasternack B. Thyroid tumors following thymus irradiation. J Natl Cancer Inst. 1985;74:1177.
-
Stovall One thousand, Weathers R, Kasper C, Smith SA, Travis 50, Ron E, et al. Dose reconstruction for therapeutic and diagnostic radiation exposures: use in epidemiological studies. Radiat Res. 2006;166:141.
-
Ron E, Lubin JH, Shore RE, Mabuchi K, Modan B, Pottern LM, et al. Thyroid cancer after exposure to external radiation: a pooled analysis of seven studies. Radiat Res. 1995;141:259.
-
The Eye Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, Ramipril, on cardiovascular events in loftier-risk patients. N Engl J Med. 2000;342:145.
-
Rothman KJ, Greenland Due south. Modern Epidemiology: second ed. Philadelphia, PA: Lippincot, Williams & Wilkins; 1998.
-
Pearson ES, Hartley HO. Biometrika tables for statisticians: third ed. London: Biometrika Trust; 1976.
-
Preston DL, Lubin JH, Pierce DA: Epicure User's Guide. In Edited by Anonymous Hirosoft International; 1991:[Bearding ].
-
Breslow NE, Mean solar day NE. Statistical Methods in Cancer Inquiry Vol 2. The Design and Analysis of Accomplice Studies: Lyon. France: International Bureau for Research on Cancer; 1988.
-
Darby SC, McGale P, Peto R, Granath F, Hall P, Ekbom A. Mortality from cardiovascular disease more than x years afterwards radiotherapy for breast cancer: nationwide cohort study of 90 000 Swedish women. Brit Med J. 2003;326:256.
-
Darby SC, Ewert M, McGale P, Bennet AM, Blom-Goldman U, Bronnum D, et al. Chance of ischemic heart illness in women later radiotherapy for breast cancer. Due north Engl J Med. 2013;368:987.
-
Mettler FA, Jr TBR, Bhargavan M, Gilley DB, Greyness JE, Lipoti JA, et al. Medical radiation exposure in the U.Due south. in 2006: preliminary results. Health Phys. 2008;95:502.
-
Little MP, Azizova Goggle box, Bazyaka D, Bouffler SD, Cardis E, Chekin Southward, et al. Systematic review and meta-assay of circulatory disease from exposure to depression-level ionizing radiation and estimates of potential population mortality risks. Environ Wellness Perspect. 2012;120:1503.
-
Yamada M, Wong FL, Fujiwara South, Akahoshi M, Suzuki One thousand. Noncancer disease incidence in atomic flop survivors, 1958-1998. Radiat Res. 2004;161:622.
-
Little MP, Kleinerman RA, Stovall K, Smith SA, Mabuchi K. Assay of dose response for circulatory affliction after radiotherapy for benign illness. Int J Radiat Oncol Biol Phys. 2012;84:1101.
-
Zablotska LB, Little MP, Cornett RJ. Potential increased run a risk of ischemic heart illness mortality with significant dose fractionation in the Canadian fluoroscopy cohort written report. Am J Epidem. 2014;179:120.
-
Lilliputian MP, Zablotska LB, Brenner AV, Lipshultz SE. Circulatory disease bloodshed in the Massachusetts tuberculosis fluoroscopy accomplice study. Eur J Epidemiol. 2016;31:287.
-
Tran V, Zablotska LB, Brenner AV, Little MP. Radiation-associated circulatory disease mortality in a pooled analysis of 77,275 patients from the Massachusetts and Canadian tuberculosis fluoroscopy cohorts. Sci Rep. 2017;7
-
Tukenova M, Guibot C, Oberlin O, Doyon F, Mousannif A, Haddy Due north, et al. Function of cancer treatment in long-term overall and cardiovascular mortality after childhood cancer. J Clin Oncol. 2010;28:1308.
-
Mulrooney DA, Yeazel MW, Kawashima T, Mertens Air conditioning, Mitby P, Stovall M, et al. Cardiac outcomes in a accomplice of adult survivors of childhood and adolescent cancer: retrospective analysis of the babyhood cancer survivor study cohort. Brit Med J. 2009;339:b4606.
-
Schultz-Hector Due south, Trott KR. Radiations-induced cardiovascular diseases: is the epidemiologic bear witness compatible with the radiobiologic data? Int J Radiat Oncol Biol Phys. 2007;67:10.
-
Darby SC, Cutter DJ, Boerma Thou, Constine LS, Fajardo LF, Kodama Thousand, et al. Radiation-related center affliction: current knowledge and future prospects. Int J Radiat Oncol Biol Phys. 2010;76:656.
-
Baselet B, Rombouts C, Benotmane AM, Baatout South, Aerts A. Cardiovascular disease related to ionizing radiations: the risk of low-dose exposure (review). Int J Molec Med. 2016;38:1623.
Acknowledgements
The authors gratefully acknowledge the data management assistance of Joe Duckett and the programming assist of Paul Winters, Eric Grant, David Richardson, and Dale Preston. We thank Emma Lipshultz for her assistance with creating the figures. The authors also give thanks the members of the accomplice and their families for standing to participate in this study. Finally, we thank Dr. Hempelmann for having the foresight to found and follow this cohort of individuals as well as his colleagues and successors who continued the surveillance of the cohort for then many years.
Funding
This study was supported past a Fellowship Grant from the James P. Wilmot Foundation, the NHLBI (Grant M-23 HL070930), and the NCI R01-CA127642. The report was likewise supported by Grant Number 5 MO1 RR00044 from the National Center for Research Resources (NCRR), a component of the National Institutes of Health (NIH) and the Academy of Rochester CTSA accolade number UL1 RR024160. The content is solely the responsibleness of the authors and does not necessarily represent the official views of the NIH.
Availability of data and materials
The de-identified data used and/or analyzed during the electric current study are available from the corresponding author on reasonable request and when a data sharing agreement has been completed.
Author information
Affiliations
Contributions
All authors have made substantial contributions to the execution of the study. MJA equally Principal Investigator was involved with all stages, from formulation and blueprint of the study to collection and assay of the data to drafting of the manuscript. All authors except MS, KTM, RGS, and RB were involved with written report conception and design. MJA, MS, AD, RB, RGS, and TAP were involved with data acquisition and interpretation of information. KTM was involved with information analysis and estimation. SGF provided input on the information analysis plan and interpretation of the results. LSC, SEL, and RES were helpful in placing the report'southward findings into context of the existing literature. MS provided master authorship of the sections on dosimetry. All authors were involved with revising the manuscript, take public responsibility for appropriate portions of the content, and have given final approval of this manuscript to be published.
Corresponding writer
Ethics declarations
Ethics approval and consent to participate
Nosotros obtained and documented bailiwick's informed consent as a function of the survey process. Report and consent procedures were canonical by the University of Rochester Research Subjects Review Lath.
Consent for publication
Informed consent was received from each participant including consent to publish aggregated findings. Copies of consent forms will exist kept for the life of the project.
Competing interests
The authors state that the proposed publication does not concern any commercial product, either straight or indirectly. All authors declare that they have no conflict of interest.
Publisher'due south Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Admission This article is distributed nether the terms of the Creative Eatables Attribution 4.0 International License (http://creativecommons.org/licenses/past/iv.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you lot give appropriate credit to the original author(southward) and the source, provide a link to the Creative Eatables license, and bespeak if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zippo/1.0/) applies to the data made available in this commodity, unless otherwise stated.
Reprints and Permissions
Almost this article
Cite this commodity
Adams, M.J., Fisher, South.G., Lipshultz, S.E. et al. Gamble of coronary events 55 Years after Thymic irradiation in the Hempelmann cohort. Cardio-Oncology four, 1 (2018). https://doi.org/10.1186/s40959-018-0027-0
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s40959-018-0027-0
Keywords
- Cardiovascular disease
- Coronary heart disease
- Childhood cancer
- Ionizing radiation
- Ischemic heart affliction
- Radiations dose-response relationship
- Radiation effects
Source: https://cardiooncologyjournal.biomedcentral.com/articles/10.1186/s40959-018-0027-0
0 Response to "Radiation Treatment in the 1950s on Babies Born With Enlarged Thymus Glands"
Post a Comment